While dentists are spared having to deal with many of the revolting maladies that physicians treat, they are not exempt from these gruesome conditions:
Gingival Myiasis
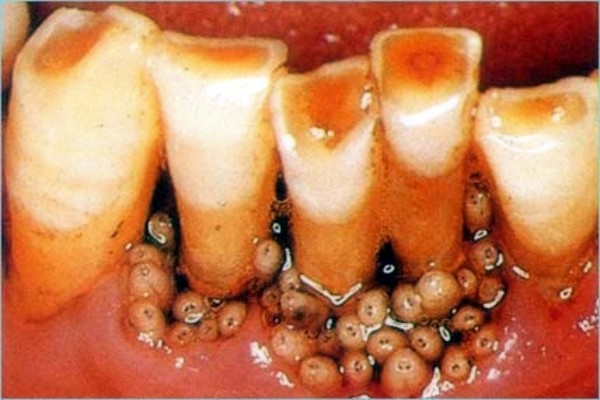
No dentist enjoys seeing generalized gross decay, but what if among the broken and rotted teeth something... squirmed?! Appallingly common in developing countries near the equator, gingival myiasis occurs when an oral area in extreme neglect is colonized by the larvae of any number of flies. The maggots, typically feeding only on dead tissue, burrow below into the gingival pockets and pupate, eventually emerging as flies. Treatment requires debridement of dead tissue, extraction of necrotic teeth, and often antibiotics to quell latent infection.
Hairy Leukoplakia
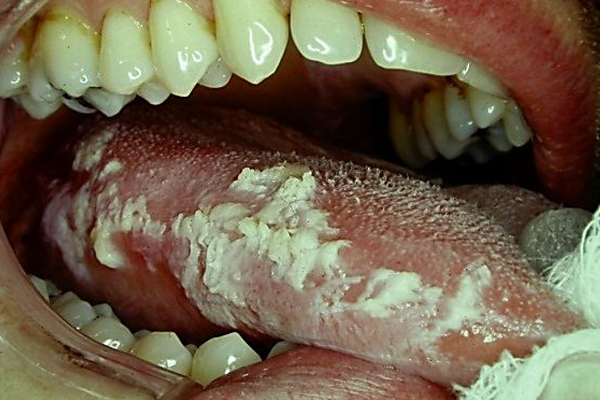
Also called “hairy tongue,” this unpleasant condition presents as whitish, keratinized tissue that can be filiform in appearance. Unlike visually similar white plaques such as pseudomembranous candidiasis, hairy leukoplakia cannot be wiped or scrubbed from the tongue, and must be treated with antiretrovirals such as acyclovir, as it caused by the Epstein-Barr virus. This condition is often an indication that an HIV+ individual has advanced to AIDS.
While certainly unsettling, this condition is self-limiting and is not precancerous. Hairy leukoplakia should not be confused with “black hairy tongue” (lingua villosa nigra), which is strongly associated with tobacco use.
Gardner Syndrome
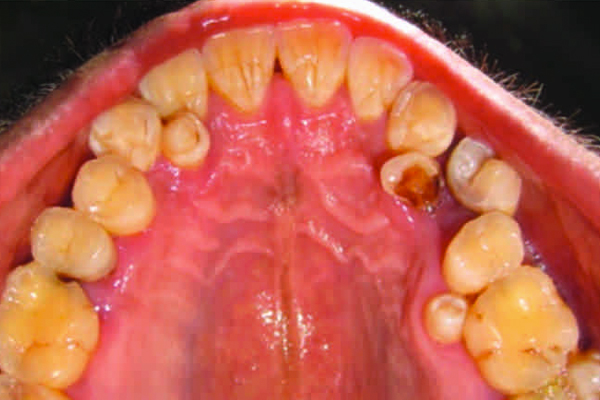
Imagine seeing a patient with nearly two rows of teeth per arch! This exceptionally rare syndrome primarily affects the colon and causes bone abnormalities. Arising from a mutation in the gene APC on chromosome 5, this mutation inactivates a key DNA repair enzyme, resulting in an increased predisposition to form adenomas in the colon and osteomas in the bone. These bone abnormalities can lead to significant numbers of supernumerary teeth! Fortunately, with proper surgical management, Gardner syndrome is not commonly fatal.
Brain Abscess Secondary to Oral Infection
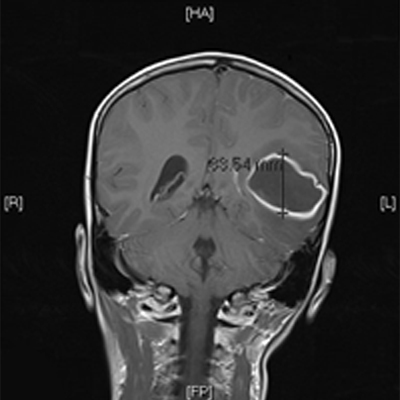
How many patients would improve their flossing habits if they knew that untreated cavities can lead to a literal hole in the brain? Throughout the medical literature there are numerous cases of this occurring, not always with obvious symptoms of infection at the site of the tooth. In one case, an 11-year-old Canadian boy was diagnosed with a 4.5cm diameter abscess secondary to a molar with gross decay. However, this molar displayed no swelling or discharge of pus, only a small radiolucency at the apex. It was only on an MRI that the brain abscess was visualized and treated with high doses of broad-spectrum antibiotics. The tooth was extracted and cultures were taken. The culprit? Streptococcus anginosus, a common oral bacterium.
Oral Teratoma
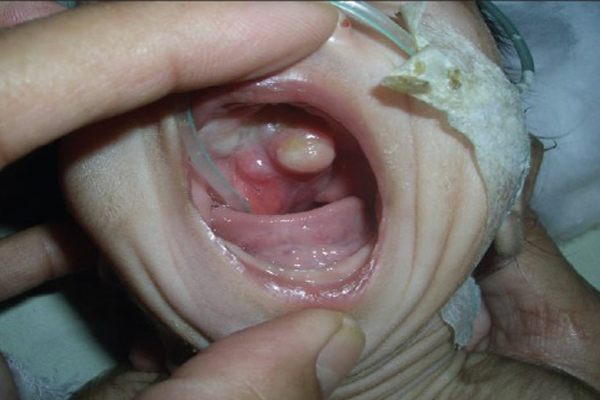
Teratomas are germline cell tumors capable of producing complex tissue including teeth, hair, muscle and more! Teratomas can grow in nearly any location, and in some cases this has included the oral cavity. In one instance featured in the International Journal of Applied and Basic Medical Research, an infant was discovered to have a palatal teratoma containing mature glial, respiratory, skin, and mucin-secreting cells. While certainly alarming, these tumors are usually not malignant, and in this case, the infant thrived as soon as the teratoma was removed.
Sources:
- Basaran, G., & Erkan, M. (2008). One of the Rarest Syndromes in Dentistry: Gardner Syndrome. European Journal of Dentistry, 2, 208–212.
- Gardner Syndrome Workup: Laboratory Studies, Imaging Studies, Diagnostic Procedures. (2017). Emedicine.medscape.com. Retrieved 24 October 2017, from https://emedicine.medscape.com/article/190486-workup
- Hairy Leukoplakia: Background, Pathophysiology, Epidemiology. (2017). Emedicine.medscape.com. Retrieved 24 October 2017, from https://emedicine.medscape.com/article/279269-overview
- Hibberd, C. (2017). Brain Abscess Secondary to a Dental Infection in an 11-Year-Old Child: Case Report | jcda. Jcda.ca. Retrieved 24 October 2017, from http://www.jcda.ca/article/c49
- Kolekar, S. S., Chincholi, T., Nangare, N., & Patankar, R. (2016). Oral teratoma. International Journal of Applied and Basic Medical Research, 6(1), 54–56. http://doi.org/10.4103/2229-516X.174015
- Kumar, S. L., Manuel, S., John, T. V., & Sivan, M. P. (2011). Extensive gingival myiasis - Diagnosis, treatment, and prevention. Journal of Oral and Maxillofacial Pathology : JOMFP, 15(3), 340–343. http://doi.org/10.4103/0973-029X.86715
The information contained in this, or any case study post in Incisor should never be considered a proper replacement for necessary training and/or education regarding adult oral conscious sedation. Regulations regarding sedation vary by state. This is an educational and informational piece. DOCS Education accepts no liability whatsoever for any damages resulting from any direct or indirect recipient's use of or failure to use any of the information contained herein. DOCS Education would be happy to answer any questions or concerns mailed to us at 106 Lenora Street, Seattle, WA 98121. Please print a copy of this posting and include it with your question or request.




